Life-threatening condition
Epidermolysis bullosa is the scientific name of a congenital skin disease that is currently considered to be incurable. Its underlying mechanism is a defect in protein-forming genes that are essential for skin regeneration. Even minor stress can result in blisters, wounds, and skin loss with scar formation. Depending on disease severity, internal organs may likewise be affected, leading to critical dysfunctions.
The disease significantly reduces the patients’ quality of life; often it is also life-threatening, as in the case of Hassan, the seven years old: by the time he was admitted to the paediatric intensive care unit at Katholisches Klinikum Bochum in June 2015, 60 percent of his epidermis was lost. “He suffered from severe sepsis with high fever, and his body weight had dropped to a mere 17 kilogrammes – a life-threatening condition,” Dr Tobias Rothoeft, Consultant at the University Children’s Hospital at Katholisches Klinikum Bochum, points out. All conservative and surgical therapy approaches failed.
First in the world: New therapy concept for large skin defects
Due to the poor prognosis, the Bochum-based team of paediatricians and plastic surgeons, in collaboration with Prof Dr Michele De Luca from the Center for Regenerative Medicine at the University of Modena, opted for an experimental therapy: the transplantation of genetically modified epidermal stem cells. Obtained from the patient via skin biopsy, these stem cells were processed in Modena. The researchers transferred the intact gene into acquired stem cells. During this process, so-called retroviral vectors were deployed, i.e. virus particles that had been specifically modified for gene transfer.
The genetically modified stem cells had been cultivated in a clean room laboratory and subsequently turned into transgenic transplants. After obtaining the parents’ permission, authorities’ approvals and certification of the operating rooms at the Bergmannsheil as genetic engineering facility, the transplantation went ahead.
Eighty percent of the body surface transplanted
At the Department of Plastic Surgery at the Bergmannsheil, the transplants were applied to the boy’s arms and legs, entire back, flanks, and partially to the stomach, neck and face as well. “Overall, 0.94 square meters of transgenic epidermis were transplanted onto the young patient in order to cover all defects, accounting for 80 percent of his entire body surface,” says Associate Professor Dr Tobias Hirsch, head consultant at the department of plastic surgery.

Group of scientists (from left): Norbert Teig (RUB/Kinderklinik), Tobias Rothoeft (RUB/Kinderklinik), Michele de Luca (Center for Regenerative Medicine, Universität Modena), Graziella Pellegrini (Center for Regenerative Medicine, Universität Modena), Tobias Hirsch (RUB/Plastische Chirurgie und Schwerbrandverletzte), Sergio Bandanza (Center for Regenerative Medicine, Universität Modena)
© CMR Unimore, Stefania Bettinelli
Following the first transplantation in October 2015, the patient’s condition began to improve. The transgenic stem cells formed a new epidermis with intact binding proteins in all transplanted areas. The integration of the intact gene through retroviral gene transfer into the genome of the epidermal stem cells had been successful and was proven to be stable.
Excellent treatment result
In February 2016, the patient was discharged. Today, almost two years after the experimental therapy was initiated, high-quality, stress-resistant skin with intact hydrolipid film, as well as early formation of hair. No scar contractures have appeared in transplanted areas. Hassan is attending school again and is actively taking part in his family’s social life.
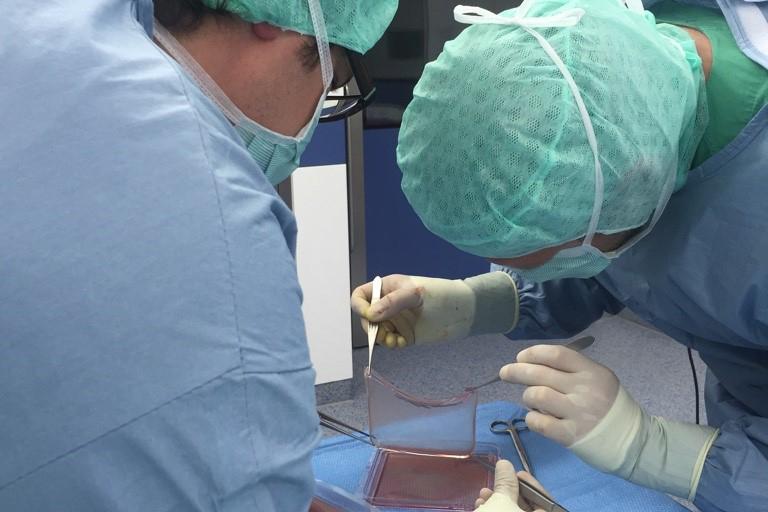
A stem cell graft is being prepared during surgery
© Frank Jacobsen
According to the international medical team, Hassan is the first patient worldwide who has been treated with skin transplants from transgenic epidermal stem cells on a large body surface area. “This approach has enormous potential for research into and development of new therapies for the treatment of epidermolysis bullosa as well as other diseases and trauma causing large skin defects” says Tobias Hirsch.
Because of its large scale, the case is considered unique on a worldwide level. “Transplanting 80 percent of the skin and providing intensive medical care to the patient over a period of eight months was extremely challenging,” Tobias Rothoeft and Tobias Hirsch point out. “The close collaboration between the departments in Bochum and the University of Modena’s expertise have been the key to success. This makes us very proud.”

The team from Bochum: Tobias Rothoeft, Tobias Hirsch und Norbert Teig (from left)
http://news.rub.de/english/press-releases/2017-11-08-worldwide-unique-boy-given-new-skin-thanks-gene...


