These new organoids can also keep cancer cells from blood cancer patients alive in the lab, something that was very difficult before. This means that doctors may now be able to test customised treatments for specific patients on their own cancer cells, to find the treatments most likely to treat the cancer.
Dr Abdullah Khan, a Sir Henry Wellcome Fellow at the University of Birmingham’s Institute of Cardiovascular Sciences and first author of the study, said: 'Remarkably, we found that the cells in their bone marrow organoids resemble real bone marrow cells not just in terms of their activity and function, but also in their architectural relationships - the cell types ‘self-organize’ and arrange themselves within the organoids just like they do in human bone marrow in the body.'
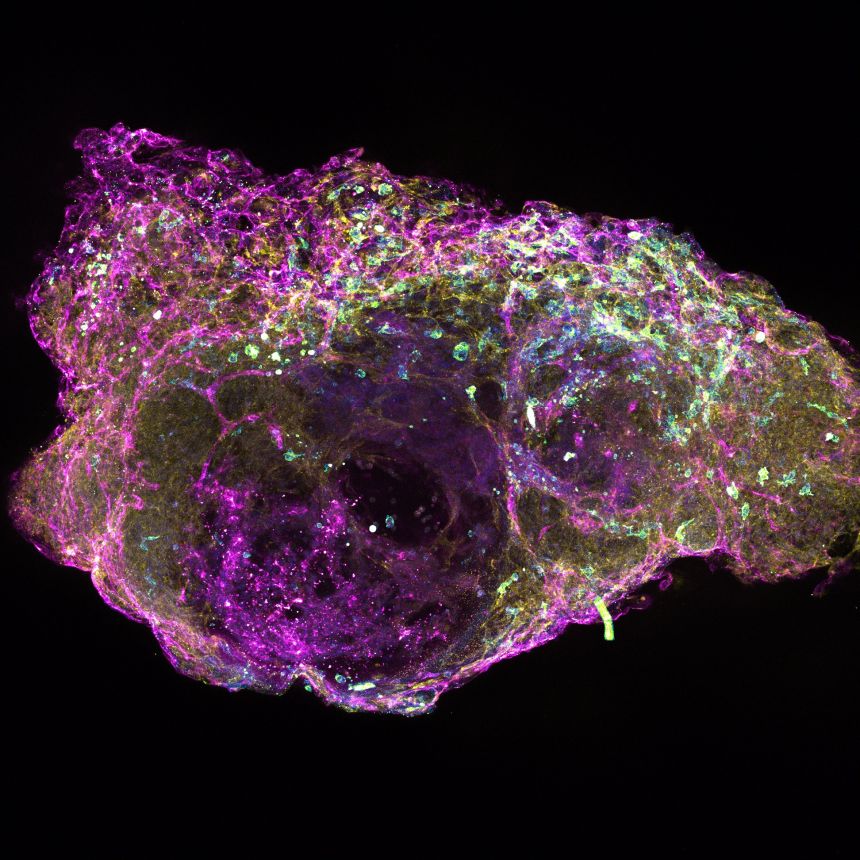
A cross section of a mini bone marrow organoids showing cells that produce blood platelets, in a network of blood vessels. Image credit: Dr A Khan, University of Birmingham
This life-like architecture enabled the team to study how the cells in the bone marrow interact to support normal blood cell production, and how this is disturbed in bone marrow fibrosis (also known as myelofibrosis), where scar tissue builds up in the bone marrow, causing bone marrow failure. Bone marrow fibrosis can develop in patients with certain types of blood cancers, and remains incurable.
Blood cancers are the most common cancers to affect children, and amongst the ten most common cancers to affect adults. In adults, they remain largely incurable.
Senior study author Professor Bethan Psaila, a haematology medical doctor as well as a research Group Leader at the Radcliffe Department of Medicine, University of Oxford, said: 'To properly understand how and why blood cancers develop, we need to use experimental systems that closely resemble how real human bone marrow works, which we haven’t really had before. It’s really exciting to now have this terrific system, as finally, we are able to study cancer directly using cells from our patients, rather than relying on animal models or other simpler systems that do not properly show us how the cancer is developing in the bone marrow in actual patients.'
Dr Khan also added: 'This is a huge step forward, enabling insights into the growth patterns of cancer cells and potentially a more personalised approach to treatment.
'Developing a protocol that enabled us to grow the organoids reproducibly and at scale was a challenge, particularly as we were working between labs in Birmingham and Oxford over the pandemic, so I spent a lot of time frantically driving organoids down the A40. However, we are thrilled with the results, as we now have a platform that we can use to test drugs on a ‘personalised medicine basis.
'Having developed and validated the model is the first crucial step, and in our ongoing collaborative work we will be working with others to better understand how the bone marrow works in healthy people, and what goes wrong when they have blood diseases.'
Dr Psaila added: 'We hope that this new technique will help accelerate the discovery and testing of new blood cancer treatments, getting improved drugs for our patients to clinical trials faster.'
The full paper, ' Human bone marrow organoids for disease modelling, discovery and validation of therapeutic targets in hematological malignancies', can be read in Cancer Discovery.


